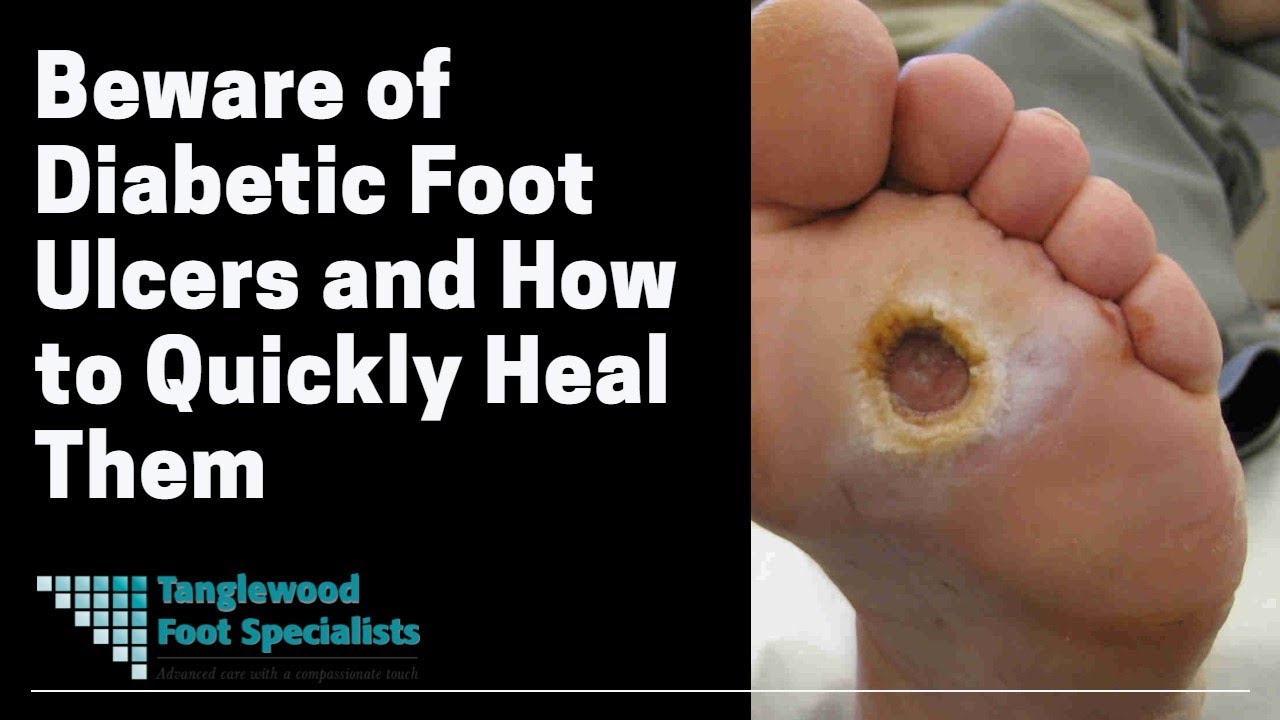
Why Diabetes and Your Feet Are a Dangerous Combination
Here's the hard truth: diabetic amputation happens when two complications — nerve damage (neuropathy) and  reduced blood flow (peripheral arterial disease) — team up to stop your body from healing foot wounds. Infections move in, tissue dies, and without intervention, limb removal becomes necessary. But according to CDC national data, over 80% of non-traumatic lower-limb amputations result from diabetes — and most were preventable with structured care.
reduced blood flow (peripheral arterial disease) — team up to stop your body from healing foot wounds. Infections move in, tissue dies, and without intervention, limb removal becomes necessary. But according to CDC national data, over 80% of non-traumatic lower-limb amputations result from diabetes — and most were preventable with structured care.
Here's what's actually happening inside your feet. Peripheral neuropathy — nerve damage caused by chronically high blood sugar — silently shuts off your foot's built-in alarm system. At the same time, peripheral arterial disease (PAD) narrows your blood vessels, cutting off the healing supply line. Think of it like a house fire with a broken smoke alarm and a blocked fire hydrant. Both problems have to exist for the disaster to happen — and with diabetes, they usually do.
That combination is what makes a blister dangerous. What heals in three days for someone without diabetes can take weeks or months when your circulation is compromised. And because the neuropathy has silenced the pain signal, you might not even know the wound exists until it's already deep. I tell every diabetic foot care patient who walks through my door the same thing: it's not the diabetes itself that causes amputations. It's what diabetes does to your ability to feel and heal.
Absence of pain is not reassurance. With neuropathy, silence is the problem.
The Five Warning Signs You Can Never Ignore
Most people with diabetic neuropathy don't experience dramatic symptoms at first — the changes are subtle, and that's exactly what makes them dangerous. The ADA Standards of Care estimates that approximately 15% of people with diabetes will develop a foot ulcer at some point in their lifetime. Knowing what to look for is the difference between catching a problem early and dealing with a crisis.
1. Numbness or tingling. Burning or tingling in your toes isn't something to sleep on — it's nerve damage in progress. Once sensation disappears entirely, a foot injury can go undetected for days. You might notice your feet feel different in the morning, or that you can't feel the texture of the floor under your socks. That's the alarm going quiet.
2. Changes in skin color or temperature. One foot noticeably warmer than the other is a clinical red flag I take seriously every single time. For lighter skin, watch for new patches of redness; for darker skin, look for areas that appear deeper or darker than usual. Any color change lasting more than 30 minutes after removing your shoes needs to be evaluated.
3. Changes in foot shape. Toes beginning to curl (hammertoe), one arch that looks flatter than it used to, or a visible change in the ball of your foot — these create new pressure points. Combined with numbness, those pressure points generate ulcers you won't feel forming.
4. A wound that isn't healing. Even a small heel crack or blister that's still open after a few days is an emergency. Don't compare your healing timeline to someone without diabetes — it's not the same biology. A wound someone else would shrug off in a week can become a serious infection in you within days.
5. Subtle infection signs. You may never get the classic fever and spreading redness that would send anyone else to the ER. Instead, watch for unexplained warmth in one area, minor swelling that comes and goes, or drainage on your socks you can't explain. Those quiet signals are your body doing the best it can to get your attention.
🚨 Get seen immediately if you notice any of the following:
- Any wound where bone is visible
- Black, purple, or gray tissue anywhere on the foot
- Red streaking moving up the leg from a wound
- Fever accompanying any foot wound
- A rapidly expanding area of redness or swelling
I won't judge you if you've been putting this off. But I need you to hear this clearly: if you have diabetes and any open wound on your foot, that wound needs to be seen today. Not this week. Today. Foot ulcer treatment is far more effective — and far less invasive — when we catch these early.
How a Houston Podiatrist Prevents Diabetic Amputation
Every case I treat follows a five-level plan — starting with the least invasive option and escalating only when necessary. What I won't do is skip levels because they take longer, or jump straight to surgery because it feels decisive. In my Houston practice, I've seen too many people told their only options were "wait and see" or amputation. There's almost always a third option — and often a fourth and fifth.
Level 1: Lifestyle and Glucose Control
 Everything else I'm about to describe depends on this foundation. Your A1C — your three-month blood sugar average — is the biological prerequisite for every other treatment. Every point your A1C rises above normal doesn't just decrease your healing ability a little. It reduces it by ten times. Not 10%. Ten times.
Everything else I'm about to describe depends on this foundation. Your A1C — your three-month blood sugar average — is the biological prerequisite for every other treatment. Every point your A1C rises above normal doesn't just decrease your healing ability a little. It reduces it by ten times. Not 10%. Ten times.
Beyond glucose control, smoking cessation is the single most impactful lifestyle change you can make for your circulation — improvements begin within weeks. Protein intake of 1.2–1.5g per kilogram of body weight daily supports tissue repair, and low-impact activity like swimming or cycling improves blood flow without adding stress to your feet. Every pound of body weight multiplies the ground force on your foot during walking, so weight management matters here too.
But here's the thing: these changes create the conditions for healing — they don't substitute for clinical care once a wound already exists. If you have any active wound or numbness in your feet, you need professional evaluation now, in parallel with making these changes. Level 1 is the engine. It doesn't replace the repair crew.
Level 2: At-Home Care
A solid daily routine can catch problems before they become wounds and slow progression that's already begun. The single most important habit is an evening foot inspection — hands on, mirror for the soles, a careful check between every toe. You're looking for anything new: a blister, a red spot, a crack, a callus that's grown.
Here's what doesn't work — and I'm being direct because these are genuinely dangerous with neuropathy. Don't use over-the-counter corn and callus removers. They contain salicylic acid, which creates chemical burns on feet that can't feel them. Don't use hot soaks or heating pads — thermal burns happen before you realize it. Don't put hydrogen peroxide or alcohol on open wounds. Both destroy the fibroblasts your body needs to build new tissue.
Diabetic-specific seamless socks, proper footwear with a wide toe box, and moisturizer applied everywhere except between the toes — these are the at-home basics that actually move the needle. But at-home care is prevention. Once a wound exists, it requires clinical management that no home routine can replace.
Level 3: Conservative In-Office Care
When you come in with an active wound, the first thing I do is stage it using the Wagner Classification — a 0–5 grading system that tells me how deep the damage goes, whether infection is present, and what tissues are involved. That staging drives every decision that follows.
Debridement is the cornerstone of everything here. Dead and damaged tissue stalls healing — it's like a construction crew that stopped working and won't let a fresh crew in. Debridement clears that out and restarts the biological cascade. I do it at every wound care visit as needed. Alongside it, offloading — eliminating all pressure on the wound — is non-negotiable. A Total Contact Cast is the gold standard for plantar ulcers; a Removable Cast Walker works well for people who can commit to keeping it on. Custom diabetic footwear and orthotics become critical once we move out of the acute phase.
I also run vascular screening using an Ankle-Brachial Index (ABI) — a simple comparison of blood pressure at your ankle versus your arm. If it shows significant PAD, I coordinate with a vascular surgeon for revascularization before wound healing can succeed. No amount of diabetic wound care works without adequate blood flow. With proper offloading and debridement, Wagner Grade 1–2 ulcers close 70–80% of the time within 12 weeks, per clinical wound research. If a wound hasn't shrunk by at least 50% after four weeks of standard care, the protocol has to advance.
Level 4: The Third Option — Advanced Regenerative Medicine
Here's what most people don't realize: there's an entire level of treatment between standard wound care and surgery. Most people never hear about it until they come to see me. I call it The Third Option — and it changes outcomes dramatically.
Skin substitutes — bioengineered tissue products — give your body the structure and cellular signals it needs to rebuild tissue it can no longer rebuild on its own. Think of them as temporary scaffolding. They don't replace your tissue permanently, but they provide the framework and growth factors that get your own cells moving again. Applied every one to two weeks when standard care stalls at the four-week mark, skin substitutes push closure rates from 70–80% all the way up to 85–95%, according to a 2023 meta-analysis. Medicare covers approved skin substitutes when specific criteria are met; most private insurance doesn't, but it's always worth checking.
Platelet-rich plasma therapy works differently. I draw a small amount of your blood, spin it in a centrifuge, and concentrate your own growth factors into a solution I inject directly into the wound margins. It's like delivering a concentrated payload of your body's own repair signals to a job site that's run out of materials. PRP carries a 70–80% success rate for appropriate candidates and costs $850 cash at TFS. Most people see a visible response within two to three weeks, across a 3–6 week series.
The combined protocol — PRP alongside skin substitutes — is the most aggressive limb-salvage approach before surgical intervention, with success rates of 85–95% over 6–12 weeks. I also use Class IV laser therapy to reduce inflammation and drive cellular repair, and shockwave therapy as additional regenerative treatments depending on the wound. One prerequisite applies to all of these: adequate blood flow. Severe PAD has to be addressed through revascularization concurrently.
If you're in Houston and dealing with a diabetic foot wound that isn't healing — or you've been told surgery might be your only option — call my office at 713-785-7881 or schedule your appointment online. The more time we have, the more options we have.
Level 5: Surgery — When It's the Right Choice
Look, I know foot surgery sounds scary. But when we're talking about diabetic foot surgery, I need you to reframe what we're actually discussing. These procedures are designed to save your foot — not remove it. Limb-sparing surgery, done well, is a success story.
The right procedure depends entirely on what's driving the problem. Surgical debridement under anesthesia removes infected tissue at a depth that office-based care can't reach. Partial ray resection removes a small bone segment or toe creating chronic pressure — it preserves the foot while eliminating the source of recurrent ulceration. Achilles tendon lengthening reduces forefoot plantar pressure by 27–30%, which is the right move when equinus deformity is driving ulcers at the ball of the foot. Charcot foot reconstruction realigns a collapsed midfoot to restore a stable walking surface. And revascularization is often the prerequisite that makes wound closure possible at any level. You can learn more about what to expect from foot surgery Houston patients specifically.
Here's what recovery looks like: non-weight-bearing in week one with close wound monitoring; protected weight bearing in a surgical boot from weeks two to four; wound closure confirmed and transition to diabetic footwear by weeks four to eight; return to modified activity with custom orthotics by months two to three. Surgery isn't failure. For the people who need it, it's the intervention that keeps them walking.
What to Expect When You Come to My Houston Practice
When you come in, I'll start by doing something that sounds almost too simple: I'll ask you to take off your shoes and socks. You'd be surprised how rarely that happens at a routine appointment. But for a diabetic patient, what I find in those first two minutes — skin color, temperature, nail condition, the shape of your arch, any callus formation — tells me more than most imaging can.
From there, I'll work through a complete lower-extremity exam. I'll test your circulation using an Ankle-Brachial Index and assess capillary refill. I'll map your sensation with monofilament testing to find exactly where feeling has diminished. If there's an active wound, I'll stage it and photograph it for tracking. And I'm going to ask about your shoes, your gait, your A1C, who's managing your diabetes, and whether you've had any previous wounds or procedures. All of that shapes the plan.
Then we'll talk about your goals. I need to know what you want to get back to — not just what your wound looks like. Some of the people I see want to walk the Memorial Park trails again. Others are trying to keep up with their grandkids or stay on their feet at work. Either way, I design the plan around where you want to be, not just around closing a wound on a chart.
You'll leave the first visit knowing exactly what we're doing, why, and what the milestones are. Wound response gets checked at two weeks and formally evaluated at four weeks for escalation decisions. I also have a free guide specifically for people dealing with foot ulcers — download it at footulcerbook.com. Either way, I need to see you — whether your wound looks serious or you're not sure it's even worth mentioning yet.
Request an Appointment →
Prevention — The Best Strategy of All
 Closing a wound is not the finish line. Up to 40% of healed diabetic foot ulcers come back within one year, according to NIH ulcer recurrence data. Closure is the halfway point. What you do after healing matters just as much as what healed it — and that means a prevention routine that runs all the time, not just when something goes wrong.
Closing a wound is not the finish line. Up to 40% of healed diabetic foot ulcers come back within one year, according to NIH ulcer recurrence data. Closure is the halfway point. What you do after healing matters just as much as what healed it — and that means a prevention routine that runs all the time, not just when something goes wrong.
Start with an annual comprehensive diabetic foot exam — Medicare covers it with a documented diabetes diagnosis. Daily evening foot inspections catch small changes before they become wounds. The Medicare diabetic shoe program covers therapeutic footwear for people with documented diabetes, and properly fitted shoes eliminate most pressure-point ulcer triggers before they start. Routine nail and callus care by a podiatrist — never at home with clippers or OTC products — removes one of the most common wound entry points. And I work closely with your endocrinologist on A1C management, because everything else depends on that number.
I see people every day who come in years into their diabetes diagnosis having never had a proper foot exam. That doesn't make them neglectful — it means nobody ever told them how important it was. Keeping up with neuropathy symptoms is what turns a dangerous condition into a manageable one. Now you know.

 reduced blood flow (peripheral arterial disease) — team up to stop your body from healing foot wounds. Infections move in, tissue dies, and without intervention, limb removal becomes necessary. But according to
reduced blood flow (peripheral arterial disease) — team up to stop your body from healing foot wounds. Infections move in, tissue dies, and without intervention, limb removal becomes necessary. But according to  Everything else I'm about to describe depends on this foundation. Your A1C — your three-month blood sugar average — is the biological prerequisite for every other treatment. Every point your A1C rises above normal doesn't just decrease your healing ability a little. It reduces it by ten times. Not 10%. Ten times.
Everything else I'm about to describe depends on this foundation. Your A1C — your three-month blood sugar average — is the biological prerequisite for every other treatment. Every point your A1C rises above normal doesn't just decrease your healing ability a little. It reduces it by ten times. Not 10%. Ten times. Closing a wound is not the finish line. Up to 40% of healed diabetic foot ulcers come back within one year, according to
Closing a wound is not the finish line. Up to 40% of healed diabetic foot ulcers come back within one year, according to