What Does a Diabetic Foot Doctor Do?
A diabetic foot doctor — typically a podiatrist — specializes in preventing, diagnosing, and treating the foot  complications caused by diabetes. These include nerve damage (peripheral neuropathy), poor circulation, foot ulcers, and infections. For people with diabetes, a podiatrist isn't just a specialist you see when something goes wrong. They're a critical member of your ongoing care team.
complications caused by diabetes. These include nerve damage (peripheral neuropathy), poor circulation, foot ulcers, and infections. For people with diabetes, a podiatrist isn't just a specialist you see when something goes wrong. They're a critical member of your ongoing care team.
Here's what makes the role different from your primary care doctor or endocrinologist. Your PCP manages your diabetes systemically — blood sugar, medications, organ function. A diabetic foot care specialist focuses entirely below the ankle, with tools your PCP simply doesn't have: monofilament testing to map exactly where protective sensation is intact, Doppler ultrasound to measure circulation, digital X-rays to catch structural changes before they become crises. It's not redundant care. It's the part of your care team that's watching the part of your body diabetes attacks first.
So here's what's actually happening in your feet when diabetes goes unmanaged at the foot level. Diabetes creates a dual threat — peripheral neuropathy removes your pain warning system while peripheral arterial disease reduces the blood flow your tissue needs to heal. Both can operate at the same time, silently, for years. I think of neuropathy like a faulty thermostat in your house: the temperature might be dangerously high — a wound, an infection, a pressure point building toward an ulcer — but the sensor is telling you everything is fine. That's why I can find a wound on the bottom of your foot that you genuinely didn't know was there.
Why Diabetes Makes Your Feet So Vulnerable
The short answer is that diabetes attacks the two systems your feet depend on most: the nerves that sense damage and  the blood vessels that repair it. High blood sugar damages nerve fibers over time, causing peripheral neuropathy — the gradual loss of your ability to feel pain, pressure, and temperature in your feet. And that same elevated blood sugar damages vessel walls, narrowing the arteries supplying your feet and reducing the blood flow that carries oxygen and healing resources to damaged tissue. The ADA Standards of Medical Care document this dual mechanism as the primary driver of diabetic lower-extremity complications.
the blood vessels that repair it. High blood sugar damages nerve fibers over time, causing peripheral neuropathy — the gradual loss of your ability to feel pain, pressure, and temperature in your feet. And that same elevated blood sugar damages vessel walls, narrowing the arteries supplying your feet and reducing the blood flow that carries oxygen and healing resources to damaged tissue. The ADA Standards of Medical Care document this dual mechanism as the primary driver of diabetic lower-extremity complications.
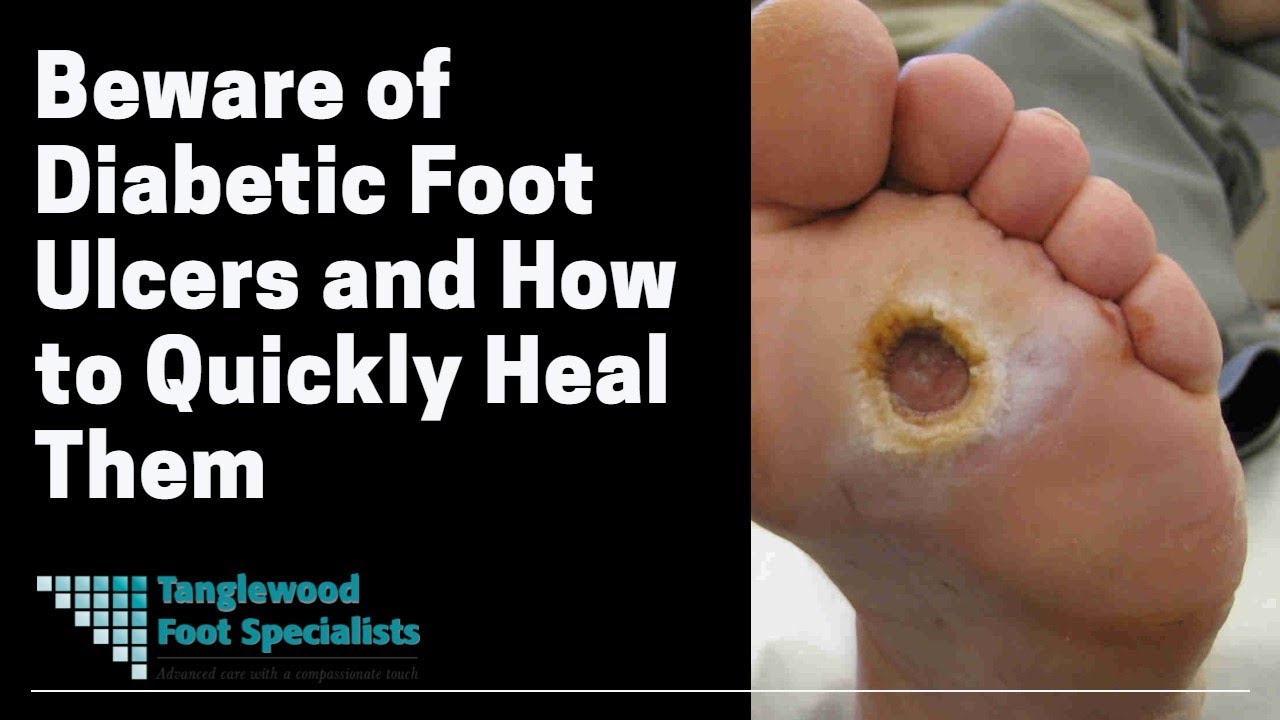
Here's what most people don't realize: every point your A1C rises above normal doesn't reduce your healing ability by 10% — it reduces it by 10 times. If your A1C is just one point too high, your healing capacity drops by 1,000%. That's not a typo. It's why a blister that would heal in three days on someone without diabetes can become a diabetic foot ulcer — an open wound where skin and underlying tissue have broken down — if it goes unnoticed and untreated. A diabetic foot ulcer carries a worse five-year survival rate than most cancers. Not because the wound itself is a death sentence, but because of what an untreated wound can become.
Contributing factors make the picture worse: poorly-fitting shoes, smoking (the single most impactful modifiable factor for circulation), high cholesterol, high blood pressure — all of them accelerate the damage. And by the time diabetic foot damage actually hurts, the nerve damage causing that pain has often been progressing for years. The people I worry about most aren't the ones who came in scared. They're the ones who didn't know they should be.
The Warning Signs You Can't Afford to Miss
I tell every diabetic patient to watch for five things: numbness without injury, skin color or temperature changes, any shift in foot shape, a cut or blister that hasn't closed in two weeks, and odor or drainage from the skin. You might notice your feet feel cold even when the room is warm, or that the skin along your toes has gone from pink to pale or bluish. You might see calluses building up in unusual spots — not just on the heel but across the ball of the foot or the side of the big toe — because your gait has been compensating for a change you haven't consciously noticed. These aren't dramatic events. They're quiet signals from a body trying to communicate through a system that's already been compromised.
Some of my patients experience the opposite of numbness — a burning, shooting pain in the feet, particularly at night. That's a different expression of the same nerve damage, and it's just as worth taking seriously. Others notice a gradual change in arch height, or that a shoe that fit well six months ago suddenly doesn't. That kind of structural shift can indicate Charcot foot — a serious complication where bones weaken and fracture under the weight of normal walking, often without pain. It looks like swelling; it gets dismissed as a sprain. I won't judge you for waiting to see if something resolved on its own. But I need you to know — with diabetic feet, hoping doesn't work.
Seek care immediately if you notice any of the following:
- Any open wound or blister that hasn't improved within 72 hours
- Redness, warmth, or swelling spreading beyond a wound's edges
- Black or darkening skin anywhere on the foot or toes
- Fever combined with any foot wound
- A sudden, dramatic change in foot shape or temperature in one foot compared to the other
These escalation criteria align with IWGDF Guidelines on diabetic foot infection assessment. A wound care podiatrist can assess all of these the same day you call. Don't wait for a scheduled appointment when these signs are present.
How a Houston Diabetic Foot Doctor Treats Your Feet
After 25 years treating diabetic patients throughout Houston — from the Galleria to the Medical Center to Tanglewood — I've built my treatment philosophy around one principle: I want to do the least necessary to get you the most durable result. That almost always means starting conservative and escalating only when the evidence demands it. Here's exactly how that progression works for my diabetic foot doctor in Houston patients.
Lifestyle Modification
Everything starts with blood sugar control — not as a lecture, but as a clinical prerequisite. If your A1C is above 7.0%, we work alongside your primary care doctor or endocrinologist to bring it down, because no wound care on earth can compensate for a healing system that's running at a fraction of its capacity. Diabetic-appropriate shoes with extra depth, a wide toe box, and Medicare-covered insoles aren't a suggestion at your first visit — they're part of the treatment plan.
And if you're a smoker, I'll be direct: nicotine constricts blood vessels, and for feet already struggling with circulation, it's the single most impactful thing you can change. Low-impact activity — swimming, cycling — combined with even a 5–10% reduction in body weight can measurably improve insulin sensitivity and reduce pressure on vulnerable tissue. These lifestyle changes take 8–12 weeks to show real impact, but they run alongside everything else from day one.
At-Home Care
Daily foot inspection isn't optional — it's the foundation that makes everything else work. I want you checking your feet at the same time every day, full surface, using a smartphone camera for the sole if you can't bend comfortably to see it yourself. Use only lukewarm water; neuropathy distorts heat perception enough that hot water can cause burns you won't feel until the damage is done.
Never use hydrogen peroxide, rubbing alcohol, or bleach on any wound. I know those feel like "cleaning" a cut, but they destroy the fibroblasts your body needs to rebuild tissue — they actively prevent healing on a diabetic foot. For minor skin care, medical-grade manuka honey is the one over-the-counter product I trust. The most important thing I can tell you about at-home care is this: it's maintenance, not treatment. Either way, I need to see you.
Conservative In-Office Care
When you come in, I start with a comprehensive diabetic foot exam — monofilament sensation testing, Doppler ultrasound and ankle-brachial index for circulation, digital X-rays, and a full skin and nail evaluation. That new patient visit runs $185 cash. From there, custom orthotics for diabetic feet are often the single most important structural intervention I can provide. Think of them like prescription eyeglasses — they compensate precisely for your specific biomechanics, redistributing pressure away from the tissue that can't protect itself. Off-the-shelf insoles don't offer that precision. Custom orthotics run $700, and for most of my diabetic patients, they're part of every visit.
High-risk patients also benefit from professional nail and callus care every 6–10 weeks ($60 cash), because a callus that builds unchecked becomes a pressure point — and a pressure point on a neuropathic foot is where ulcers begin. For active wounds, I use sharp debridement, advanced wound dressings, and total contact casting or offloading. Removing all pressure from the wound site is the single most critical mechanical intervention for diabetic ulcer healing. Standard wound care closes 70–80% of ulcers. But according to IWGDF wound care guidelines, if your wound hasn't reduced in size by at least 50% at the four-week mark, that's the trigger to advance treatment — not a reason to keep waiting.
Advanced Regenerative Medicine — The Third Option
Most people don't know this level of care exists. There's a full tier of treatment between standard wound care and surgery — and it's where I see the most dramatic results for people who'd been told their options were running out.
Platelet-rich plasma therapy — platelet rich plasma therapy, or PRP — is drawn from your own blood, concentrated in a centrifuge to isolate growth factors and platelets, then applied directly to a stalled wound. Think of a diabetic ulcer that won't close like a construction crew that started the job and got stuck. PRP brings the crew back and gives them the tools to finish. A systematic review in the International Wound Journal found PRP significantly improved healing rates in chronic diabetic foot ulcers compared to standard care alone. Cash cost is $850 per session.
For wounds that need structural support to regenerate, I use bioengineered skin substitutes — temporary scaffolding that gives your body the biological framework it needs to grow new tissue. The Liposana amniotic allograft I use most frequently runs $975 per vial. Medicare does cover approved skin substitutes when specific criteria are met; most private insurance does not. I also use red light therapy for tissue healing as an adjunctive treatment to support circulation — $39 per session, or $180 for a six-pack. The difference these regenerative medicine options make is measurable: standard wound care closes 70–80% of ulcers; with advanced regenerative protocols, that number climbs to 85–95%.
There's also fat pad restoration for people whose protective tissue has thinned under high-pressure areas — a tool that can reduce ulcer risk before a wound ever develops.
Surgery — When It's Necessary
Look, I know foot surgery sounds scary — especially when you've already been warned about the risks of diabetic healing. But every step above this line exists because I want to keep you out of this one. The 154,000 diabetic amputations performed in the U.S. each year aren't failures of medicine. Most are failures of early intervention — and research shows that having a podiatrist actively involved in your care reduces your amputation risk by 36%. The people I worry about aren't the ones sitting in my chair. They're the ones who are waiting.
When surgery is the right answer, I use the most targeted approach the situation allows. Debridement and drainage for a deep infection or abscess is outpatient, under local anesthesia, and most people are back to protected weightbearing within days. If MRI confirms osteomyelitis — bone infection that develops when a wound penetrates deep enough to reach bone — surgical removal of the infected bone may be necessary, with recovery running 1–2 weeks non-weightbearing, then 3–6 weeks in a surgical boot, then a graduated return to normal footwear. When Doppler testing confirms arterial blockages preventing wound healing, I coordinate directly with vascular surgery colleagues for revascularization before advancing wound treatment. For anyone who needs foot surgery, I'll walk you through every detail before we schedule anything.
Not Sure If You Need to Come In?
If your wound hasn't closed in two weeks, the answer is yes. Call 713-785-7881.
Request an Appointment
What to Expect at Your First Diabetic Foot Visit
When you come in, I'll start with a full neurological and vascular assessment before we talk about anything else. I'll use a monofilament — a thin filament pressed against different points on your sole — to map exactly where protective sensation is intact and where it isn't. Then I'll run a Doppler ultrasound and ankle-brachial index to measure how well blood is reaching your feet, comparing pressure at the ankle to pressure at the arm. Digital X-rays follow, so I can evaluate bone structure, look for early Charcot changes, and assess any structural deformities contributing to pressure buildup.
I'm also going to look at your shoes. I'll ask when you last replaced them, how long you're on your feet each day, and what your daily inspection routine looks like — without judgment, because most people haven't been taught one. If you have an active wound, you won't leave with "let's watch it." You'll leave that same visit with a treatment plan and initial wound management already in place. The full new patient exam runs 45–60 minutes.
After your first visit, we'll set a monitoring schedule based on what we find. Stable patients with no active complications typically come in every 6–12 months. If you have neuropathy or a history of ulcers, I want to see you at least every 6 weeks. An active wound gets as much attention as it demands — weekly visits aren't unusual. Either way, I need to see you — whether you have a wound right now or you're trying to make sure you never do. Request your appointment and we'll figure out exactly where you stand.
Protecting Your Feet Long-Term: What Houston Diabetics Need to Know
Houston's heat and humidity create conditions that accelerate exactly what diabetic feet are most vulnerable to. Shoes trap moisture against compromised skin. Sidewalks and patios in August stay hot enough to cause burns that neuropathic feet will never feel. And the heavy protective footwear some people rely on is genuinely difficult to wear for a full day in our climate. I tell my patients near the Galleria and across the Medical Center the same thing: the solution isn't to avoid activity — it's to build daily foot inspection into your routine the same way you'd check your blood sugar.
The annual exam is a floor, not a ceiling. In Houston's heat, your shoes need time to fully dry between wearings — rotating between at least two pairs isn't optional, it's basic skin protection. Up to 40% of healed diabetic ulcers recur within one year, so ongoing monitoring isn't a sign that something went wrong. It's the standard of care for a condition that doesn't take breaks. Neuropathy management and Class IV laser therapy are both tools I use to support nerve function and circulation between acute episodes — not just reactive care, but ongoing protection. My free resource at diabeticfootbook.com is a good place to start if you want a deeper guide to daily diabetic foot care.

 complications caused by diabetes. These include nerve damage (peripheral neuropathy), poor circulation, foot ulcers, and infections. For people with diabetes, a podiatrist isn't just a specialist you see when something goes wrong. They're a critical member of your ongoing care team.
complications caused by diabetes. These include nerve damage (peripheral neuropathy), poor circulation, foot ulcers, and infections. For people with diabetes, a podiatrist isn't just a specialist you see when something goes wrong. They're a critical member of your ongoing care team. the blood vessels that repair it. High blood sugar damages nerve fibers over time, causing
the blood vessels that repair it. High blood sugar damages nerve fibers over time, causing