Even in Houston, winter can be a difficult season for people with diabetes. Temperature drops and drier air dry out your feet. And snug boots can rub or pinch, causing blisters and making bunions more painful. In so many ways, this time of year can attack your feet. So, today we'll look at each problem. Then, we'll offer you tips to keep the cold from hurting your feet.
Cold Weather and Diabetic Neuropathy

Here's one seasonal worry you might not know about. It's harder to manage peripheral neuropathy in cold weather. (This is a condition that makes you lose feeling in your extremities. It could also trigger burning pain in your feet. Some people even say it makes them feel like their feet are stuck in wax.)
Whatever your symptoms, it's harder to stop neuropathy complications when it's cold. And that's because of a few different reasons.
In the cold weather, you tend to keep your feet covered more often; this is natural, since you want your feet to stay warm. ( After all, poor circulation makes your feet even colder than other people’s. So choosing warm socks is a much safer option than putting your feet near a space heater. You should also avoid heating pads. Or dipping feet in hot water. These are all risky choices if you have neuropathy. Because you could burn yourself in your struggle to warm up, since you may not feel dangerously-hot temperatures.)
Unfortunately, this cover up could spell trouble. If you don’t feel your feet well, and you aren’t looking at them frequently, you can easily overlook a small injury. As a result, you could miss the early stages of infection. And a small injury could develop into a dangerous ulcer.
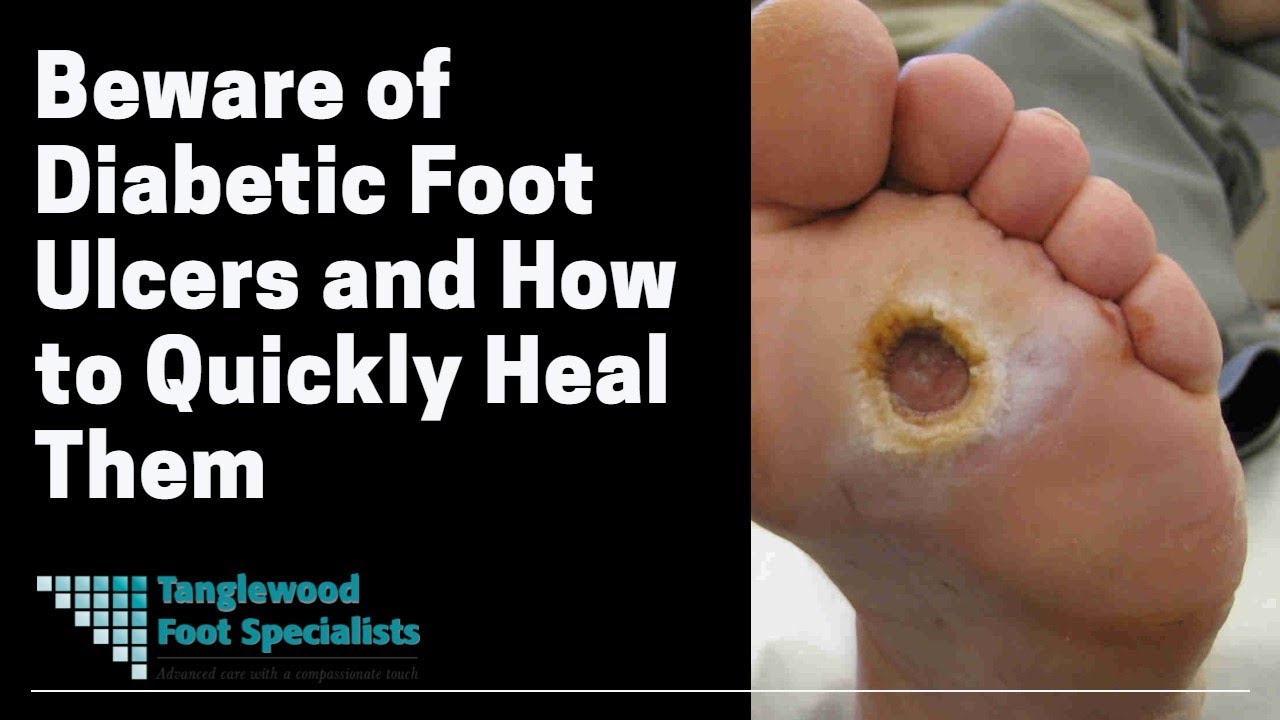
And the problems get worse. Ulcers can form anywhere. But some of the more common places are on the ball of your foot or on the bottom of your big toe. And, if your feet are always covered by heavy socks or stuffed into large winter boots, you can easily develop a callus in one of those places.
Now, if you notice a callus quickly, I can help you manage the hard skin and prevent complications. But if you keep that toe covered and don't see the problem? That spells trouble. Because, without proper care and attention, calluses can become infections. And that can lead to further diabetic foot complications.
Cold Feet Could Mean Neuropathy
Just to make things more complicated, if your feet are cold this winter, it could be the temperature drop. But it could also mean you're developing neuropathy. In fact, if your feet are cold, and you also feel a burning sensation, it's very likely that you're experiencing the nerve pain associated with neuropathy. Other symptoms may include weakness or numbness.
Even if your cold feet aren't a sign of neuropathy, that doesn't mean you should just layer on the socks and wait for warmer weather. Chronically cold feet are also a symptom of Reynaud's disease and anemia, so it's worth getting a check up if your feet always feel chilled. Then, if it turns out neuropathy is the source of your chill, we can help you feel better using the latest treatment protocols.
Updated Guidelines for Treating Painful Neuropathy
Recently, the American Academy of Neurology issued updated neuropathy treatment guidelines. It's the first update since 2011. And it can help you protect your diabetic feet in winter, and all year long.
The guidelines say that certain medications could now reduce nerve pain. These newer options include tricyclic anti-depressants (TCAs), and SNRIs. ( Serotonin-norepinephrine reuptake inhibitors.) They join traditional options, like gabapentinoids and sodium channel blockers. And the new guidance suggests trying one class of medication, then moving to a different option if pain doesn't go away.
Neuropathy Care in Houston, TX ![Winter boots can give diabetic feet calluses]()
I always follow the latest recommendations from trusted medical groups. But I also have other ways to manage peripheral neuropathy in my Houston podiatry practice.
First of all, I'll always work with you to help you control your diabetes. This will help prevent neuropathy from getting worse. Whether that's by offering diabetic meal planning help, or connecting you with other care team members, I'm here to help.
I also focus on adding nutrition to your diet. In fact, one of the most exciting neuropathy therapies focuses entirely on nutrition. What do I mean? I'm talking about Neuremedy. It's a bioactive form of Vitamin B1. And many diabetics say it relieves their neuropathy pain and numbness. All by by providing your body with the appropriate nourishment.
Other Winter Safety Tips for Diabetic Feet
Now we've covered why you need to manage neuropathy. (And offered new ways to help you do that.) But let's look at other ways you can avoid winter setbacks and keep your feet healthy.
First up? Inspect your feet at least twice a day, if not more often, even if it means letting them get cold for a minute or two. During the rest of the year, I'm ok with one home-foot exam each day. But since your circulation gets worse in winter, and your feet are less visible, adding an extra check is important. (Here's how to conduct a thorough home foot exam for diabetics.) Next on my list? Get regular exercise. After all, working out is a great way to warm up and improve your circulation without risking burns. Plus, regular exercise can help you get to or stay at a healthy weight. And, since weight loss may prevent diabetic complications, this tip is a win on all fronts. Finally, I want you to focus on stepping up your moisturizing routine. Here's the deal. Your skin is naturally dryer during the winter months. Add in dry air because you finally turned your home heat on? Suddenly, you've got a recipe for cracked, bleeding skin on your feet.
Lotions and Creams for Diabetic Foot Protection
During warm and humid months, you may be able to use a thinner mositurizing lotion. But in the winter? I want my diabetic patients to stick with creams. (They're thicker moisturizing agents.)
Usually, an over-the-counter cream like Eucerin or Cetaphil offers great protection. But if I'm really worried about your feet cracking, I'll recommend something stronger. Often, that means I'll look for a cream that contains urea. This ingredient is a natural moisturizer. It also pulls water into your skin and keeps it there. Which is why, if your feet are very dry, I'll recommend a product with at least 20% urea content.
What else can I say to help your diabetic feet stay safe this winter?
Stay vigilant! At the first sign of any foot infection, call Dr. Andrew Schneider for an immediate office visit.